Paula is vijftien kilo te zwaar en probeert al jaren af te vallen. Ze heeft talloze diëten gevolgd, allemaal zonder succes. Overdag op haar werk gaat het goed. Maar zodra de kinderen ’s avonds in bed liggen en de televisie aan gaat, dan gaat het mis. Het lijkt alsof haar lichaam schreeuwt om die chocolade in de kast. Cue exposure therapie helpt haar lichaam de mond te snoeren. ‘Het is voor de klinische praktijk van belang om zoveel mogelijk essentiële voedingsmiddelen te betrekken tijdens cue exposure therapie,’ stelt Ghislaine Schyns.
Paula heeft overgewicht, en ze is niet alleen. In 2016 had bijna de helft van de volwassen Nederlandse bevolking overgewicht (Body Mass Index (BMI) > 25), en bij veertien procent van de Nederlanders was er sprake van obesitas (BMI > 30) (CBS, RIVM & Trimbos-instituut, 2016)11. Overgewicht en obesitas gaan niet alleen gepaard met ernstige lichamelijk aandoeningen, zoals cardiovasculaire ziekten en diabetes, maar hebben ook negatieve gevolgen voor de kwaliteit van leven, onder meer door gewichtsdiscriminatie en mobiliteitsproblemen (Finer, 2015; Uzogara, 2017)1631. Ondanks dat mensen massaal proberen af te vallen, lukt dit maar enkelen: volgens schattingen slaagt slechts twintig procent van de mensen met overgewicht erin om minimaal tien procent gewichtsverlies te bereiken én om dit gewichtsverlies er langer dan een jaar vanaf te houden (Wing & Phelan, 2005)37.
De toename in overgewicht in de afgelopen decennia hangt samen met de grote overvloed van eten dat overal te koop is. Onze ‘obesogene’ omgeving zit vol met triggers om te gaan eten, en zet ons zelfs aan tot eten wanneer we geen echte honger hebben. In deze obesogene omgeving zijn het de voedsel-geassocieerde cues die ons aanzetten tot eten, zoals het zien van de Italiaanse ijstent, of de geur van versgebakken wafels in de winkelstraat. Waarneming van dergelijke cues zorgt ervoor dat ons lichaam zich alvast gaat voorbereiden op voedselinname, bijvoorbeeld door extra speeksel te produceren, insuline en ghreline aan te maken, en trek te ervaren. Deze verzameling van reacties wordt cue reactiviteit genoemd. Ondanks dat cue reactiviteit een normale reactie is, blijkt de reactiviteit beduidend groter te zijn bij mensen met overgewicht dan bij mensen met een normaal gewicht (Ferriday & Brunstrom, 2011)15. Sterker nog, uit een recente meta-analyse blijkt dat de verhoogde reactiviteit een centrale rol speelt in overgewicht, aangezien cue reactiviteit een significante voorspeller is voor overeten en gewichtstoename (Boswell & Kober, 2016)5. Verhoogde cue reactiviteit zou het volhouden van een dieet behoorlijk kunnen belemmeren. Dit bleek inderdaad het geval te zijn op basis van resultaten van een pilotstudie, waarin cue reactiviteit werd gemeten bij succesvolle en niet succesvolle lijners (Jansen et al., 2010)25. De niet succesvolle lijners hadden op het moment van deelname nog steeds obesitas, ondanks serieuze lijnpogingen, en de succesvolle lijners hadden op het moment van deelname een gezond gewicht na voorheen obees te zijn geweest. De resultaten lieten zien dat de succesvolle lijners minder cue reactief waren dan de onsuccesvolle lijners. Het zou dus zo kunnen zijn dat cue reactiviteit vermindert als iemand een tijdje geen lekkere snacks eet. Verminderende cue reactiviteit kan het ook weer makkelijker maken om van snacks af te blijven, en kan daarmee succesvol gewichtsverlies bevorderen (Jansen, 1998; Jansen, Havermans, & Nederkoorn, 2011)2123.
Trek in chocolade door een muziekdoos
Leertheoretische modellen suggereren dat cue reactiviteit voor een belangrijk deel kan worden aangeleerd (Jansen, 1998; Jansen et al., 2016)24. Wanneer bepaalde cues een aantal keren gepaard gaan met inname, kan er een cue-voedselinname associatie ontstaan. Bij een sterke cue-voedselinname associatie is enkel de blootstelling aan de cue voldoende om cue reactiviteit aan te wakkeren.
Associaties leggen tussen cues en eten blijkt gemakkelijk te gaan, zo blijkt uit studies uit ons laboratorium in Maastricht. In een conditioneringsexperiment kregen proefpersonen bijvoorbeeld twee muziekdoosje te zien: een blauw muziekdoosjes en een wit muziekdoosje. In de aanleerfase kreeg iedere proefpersoon telkens één van beide doosjes te zien, één doosje tegelijk. Enkel bij het zien van het blauwe doosje kreeg de proefpersoon telkens een stukje chocolade, het witte doosje bleef onbeloond. Na enkele blauwe-dooschocolade- herhalingen rapporteerden proefpersonen bij het zien van het blauwe doosje een verhoogde trek, vergeleken met de trek bij het zien van het witte doosje. Proefpersonen leerden dus trek in chocola te krijgen bij het zien van een muziekdoos.
Interessant is dat deze geconditioneerde trek aan te leren valt met velerlei neutrale stimuli, zoals vaasjes met bloemen, dienbladen en tijdstippen (Van den Akker, Havermans & Jansen, 2017; Bongers, Jansen, 2017; Bongers et al., 2015; Van den Akker et al., 2014; Van den Akker, Havermans, & Jansen, 2015; Van den Akker et al., 2013)134323334. In het dagelijks leven maken we associaties met cues met een extern karakter, zoals het zetten van een kop koffie, het terugkomen van het werk, of het aanzetten van de televisie. In het voorbeeld van Paula zal het herhaaldelijk eten van een stuk chocolade tijdens het televisiekijken in de avond ertoe leiden dat een sterke associatie wordt gevormd tussen de televisie en het eten van chocolade. Als gevolg zal enkel de presentatie van de cue, het aanzetten van de televisie, zorgen voor een geconditioneerde trek in eten. Naast externe cues, zijn we ook in staat om associaties te leggen met interne cues, zoals gevoelens van vermoeidheid of somberheid. Wanneer Paula tijdens haar snackmoment ook altijd sterk vermoeid is, zal er dus ook een link ontstaan tussen vermoeidheid en het eten van chocolade.
Extinctie van aangeleerde trek
Wanneer we ervan uitgaan dat cue reactiviteit een aangeleerde respons is, kunnen deze geconditioneerde reacties worden verminderd volgens het principe van extinctie. Tijdens extinctie worden voedsel-geassocieerde cues aangeboden, zonder dat deze worden gevolgd door het consumeren van voedsel. Na een aantal herhalingen neemt de geconditioneerde reactie af. Aanvankelijk werd het afnemen van de geconditioneerde respons geweten aan het vernietigen van de cue-voedselinname-associatie. Onderzoek van Bouton en collega’s heeft evenwel aangetoond dat de originele associatie blijft bestaan, en naast de originele associatie tijdens extinctie een nieuwe inhibitoire associatie word gevormd, namelijk cue-geen voedselinname (Bouton, 1993; Bouton & King, 1983)89. De cue krijgt dus als het ware twee betekenissen: cue-voedselinname én cue-geen voedselinname. Hoe sterker de inhibitoire cue-geen voedselinname- associatie, hoe sterker de afname van de conditioneerde reactie. Cue exposure therapie is de klinische vertaling van extinctieleren: de patiënt wordt herhaaldelijk blootgesteld aan de voedsel-geassocieerde cues, zoals het zien, voelen en ruiken van voedsel, terwijl de consumptie van eten niet is toegestaan.
In kleinschalige studies blijkt cue exposure-therapie goed te werken voor bulimia nervosa-patiënten. Zo werd in een studie bij 22 bulimia nervosa-patiënten die niet opknapten door de reguliere behandeling cue exposure therapie ingezet. Direct na afloop van therapie, maar ook na zes maanden follow-up, waren de eetbuien bij deze patiënten sterk gereduceerd (Martinez-mallen et al., 2007)28. Tijdens een eetbui wordt er een ongewoon grote hoeveelheid voedsel binnen een relatief korte tijd gegeten, waarbij er controleverlies wordt ervaren (American Psychiatric Association, 2013)2. Overigens zijn eetbuien ook een veelvoorkomend probleem bij obesitas (Marcus & Wildes, 2009; Mustelin et al., 2017)2730. In een andere pilotstudie leidde cue exposure-therapie zelfs tot een complete stop van eetbuien na afloop van therapie, en dit effect bleef behouden na één jaar follow-up (Jansen, Broekmate, & Heymans, 1992)22.
Effecten van cue exposure bij overgewicht werden tot nu toe nauwelijks onderzocht, en we hebben geen kennis over de werkingsmechanismen. Voor de toepassing voor overgewicht zijn er dus veel prangende vragen, zoals de vraag of cue exposure-therapie ook kan helpen om succesvol gewichtsverlies te kunnen bereiken. Een onderzoek door Mount en collega’s (1990) doet vermoeden van wel. In dit onderzoek kregen proefpersonen na afloop van een intensief afvalprogramma een therapie om terugval in gewicht te voorkomen: ofwel cue exposure-therapie, ofwel een stimulus controle interventie waarin proefpersonen in feite leerden om voedselcues te ontwijken. Uit de resultaten bleek dat proefpersonen die cue exposure-therapie hadden ontvangen het gewichtsverlies hadden weten te behouden na een periode van vier maanden, in tegenstelling tot de proefpersonen in de stimuluscontrole-interventie (Mount et al., 1990)29. In een meer recent onderzoek kregen obese vrouwen met eetbuiproblemen een interventie waarin cue exposure-elementen waren verwerkt, en deze groep bleek een iets lagere te hebben na veertien sessies therapie (minder dan één -punt), ook na drie maanden follow-up (Boutelle, Knatz, Carlson, Bergmann, & Peterson, 2016)6.
Bovenstaande studies geven echter geen bewijs dat cue exposure-therapie inderdaad werkt om af te vallen en bovendien was de reductie in kilo’s beperkt. Een belangrijke afgeleide van gewichtsverlies is het minder ‘overeten’ van hoogcalorische producten. Immers, het binnenkrijgen van energie zonder dat daartoe een fysieke behoefte bestaat, maakt dat overtollige energie wordt opgeslagen in vet, en dat resulteert dus in gewichtstoename. Onderzoek laat inderdaad zien dat eten van hoogcalorische snacks, zonder dat proefpersonen echte honger hebben, samenhangt met de ernst van obesitas (Butte et al., 2007; Kral et al., 2013)1026. Eten van snacks zonder honger werd als uitgangspunt genomen in een onderzoek naar cue exposure-therapie bij obese kinderen (Boutelle et al., 2011)7. In dit onderzoek werden proefpersonen ingedeeld in een cue exposure-interventie waarbij kinderen acht sessies cue exposure-therapie kregen, of in een interventie waarin kinderen leerden om verzadigingssignalen te herkennen. Kinderen in de cue exposuregroep aten minder snacks na afloop van cue exposure dan kinderen in de alternatieve interventie, hoewel deze reductie zich niet vertaalde in gewichtsverlies.
Samengevat is cue exposure-therapie een potentieel effectieve interventie om overeten en gewichtsverlies te bevorderen, al zijn er maar weinig studies die de effecten van cue exposure-therapie in een (volwassen) obese populatie hebben onderzocht. Samen met collega’s heb ik daarom in een aantal experimentele studies onderzocht of cue exposure inderdaad werkt om overeten en lichaamsgewicht te reduceren.
In een eerste experiment werden 54 vrouwen met overgewicht en obesitas ingedeeld in een cue exposure-conditie of in een actieve controle-conditie. Proefpersonen in de cue exposure-conditie kregen één sessie cue exposure-therapie met vier van hun persoonlijk favoriete voedingsmiddelen. Proefpersonen werden tachtig minuten lang geïnstrueerd om de drang om te eten zo hoog mogelijk op te voeren, door het eten vast te pakken, te ruiken, te breken, te likken, maar niet op te eten. Naast de vier persoonlijke voedingsmiddelen kreeg iedere proefpersoon ook een bakje chocolademousse op hun dienblad voor de exposure-oefeningen. Na afloop van de sessie kregen de proefpersonen eerst een dubbele sandwich zodat ze geen honger meer hadden, en kregen ze vervolgens een zogenaamde ‘smaaktest’. Tijdens deze smaaktest kreeg iedere proefpersoon zes smakelijke toetjes voorgeschoteld (zie figuur 1), waarvan zij mocht aangeven wat ze van de smaak van ieder toetje vond door goed te proeven. De instructie voor deze smaaktest was dat de proefpersoon tien minuten de tijd kreeg om de smaken te beoordelen met behulp van een vragenlijst, terwijl ze zoveel van de toetjes mocht eten als ze zou willen. In tegenstelling tot het gecommuniceerde doel naar de proefpersoon, waren wij enkel geïnteresseerd in de gegeten kilocalorieën, en wel toegespitst op twee categorieën van voedingsmiddelen: de blootgestelde en niet-blootgestelde voedingsmiddelen. De chocolademousse vormde het blootgestelde voedingsmiddel, en de overige vijf toetjes fungeerden als niet-blootgestelde voedingsmiddelen.
In vergelijking met de controleconditie, waarin proefpersonen psycho-educatie kregen over een gezonde leefstijl en lichaamsbeeld, aten de proefpersonen in de cue exposureconditie beduidend minder kilocalorieën van chocolademousse, het blootgestelde voedingsmiddel. De hoeveelheid die gegeten werd van de niet-blootgestelde voedingsmiddelen was echter niet verschillend tussen de condities, wat betekent dat het effect van één sessie cue exposure-therapie niet generaliseerde naar andere voedingsmiddelen die niet tijdens cue exposure aan bod waren gekomen.
Effect van cue exposure op overeten
De resultaten van de bovenstaande studie impliceren dat cue exposure overeten vermindert, althans voor blootgestelde voedingsmiddelen. Zou het generaliseren naar niet-blootgestelde producten wél optreden bij meer dan één cue exposure-sessie? De vraag of cue exposure-effecten generaliseren is belangrijk voor de vertaling van deze resultaten naar de klinische praktijk. Namelijk, is het voldoende om slechts enkele voedingsmiddelen in de cue exposure-sessies te betrekken, zodat de patiënt profijt zal hebben bij een breder scala aan voedingsmiddelen? Of is het van belang om zoveel mogelijk voedingsmiddelen te betrekken tijdens cue exposure-therapie om zo voldoende zoden aan de dijk te zetten voor succesvol gewichtsverlies?
Wij boden een uitgebreidere vorm van cue exposuretherapie aan achttien vrouwen met gewichtsproblemen aan, en vergeleken deze groep met een groep van twintig vrouwen die een controle-interventie ontving, gericht op een gezonde leefstijl. Voordat deelneemsters volgens het lot werden ingedeeld in één van beide interventies, kregen ze eerst een uitgebreid interview. Tijdens dit interview werden nauwkeurig alle relevante cues in kaart gebracht die de proefpersoon associeerde met overeten (denk bijvoorbeeld aan de televisie en vermoeidheid van Paula), al dan niet in de vorm van eetbuien. Daarnaast werden ook de ‘problematische’ snacks in kaart gebracht, dat zijn hoogcalorische producten die regelmatig betrokken waren bij overeet-episodes én waarmee controleproblemen werden ervaren. Naast deze individuele snacks selecteerde iedere proefpersoon ook de lekkerste snack uit een standaardlijstje van tien producten (zoals chocolade, koekjes en chips). Deelnemers in cue exposure-interventie ontvingen acht sessies cue exposuretherapie en deden daarnaast gemiddeld 28 huiswerk exposures binnen een periode van één maand, met zowel de individueel geselecteerde snacks als de snack uit de standaardlijst. Eén van de individuele snacks werd bewust buiten de exposure-oefeningen gehouden, ter wille van de smaaktest aan het einde van de therapie. Deze niet-blootgestelde individuele snack werd meegenomen in de smaaktest, alsook één individuele snack die wel werd gebruikt tijdens de exposure-oefeningen, en de standaard snack die ook aan bod kwam tijdens cue exposure.
De resultaten steunden deels onze hypothese: van de blootgestelde individuele snack werd, zoals in eerder onderzoek, significant minder gegeten in de cue exposureconditie dan in de controleconditie. Maar van de blootgestelde standaard snack werd niet meer of minder gegeten dan in de andere conditie. Dit laatste is bijzonder, omdat het aantal exposure-oefeningen per snack nauwkeurig werd bijgehouden gedurende sessies en huiswerkopdrachten, en gelijk bleek te zijn voor de individuele en standaardsnack. Gemiddeld deed een proefpersoon zeven tot acht exposureoefeningen met de individuele én de standaardsnack, desondanks hadden deze exposures een minder sterke invloed op consumptie van de standaard snack. Cue exposure blijkt dus inderdaad effectief overeten te verminderen van blootgesteld voedsel, maar vooral voor voedingsmiddelen die controleverlies uitlokken en niet zozeer voedingsmiddelen die ‘gewoon lekker’ zijn. Voor de behandelaar is er dus werk aan de winkel; het is niet voldoende om een willekeurige reep chocolade uit de automaat te trekken voor een cue exposure-sessie. Voorafgaande aan cue exposure is per individu een grondige inventarisatie van de specifieke problematische voedingsmiddelen gewenst. De resultaten van de smaaktest waren niet alleen verassend wat betreft de blootgestelde standaardsnack, maar ook wat betreft de niet-blootgestelde individuele snack: geen verschil tussen de condities. Dus zelfs na een flink aantal cue exposure-sessies en huiswerkopdrachten binnen een korte periode van één maand blijken cue exposure-effecten niet te generaliseren naar andere voedingsmiddelen.
Het niet-vinden van generalisatie van exposure-effecten lijkt echter niet specifiek te zijn voor cue exposure-therapie; generalisatie na exposure-therapie is ook een probleem in andere onderzoeksgebieden. Van den Hout en collega’s (2011)35 onderzochten bijvoorbeeld het effect van exposure-therapie voor smetvrees. 65 smetvrees-gevoelige proefpersonen ondergingen twee exposure-sessies met één potentieel vuil voorwerp, zoals een schoenzool of een prullenbak met afval. Na afloop van de sessies rapporteerden proefpersonen minder gevoelens van besmetting, gevaar, angst en walging voor het voorwerp dat tijdens de exposureoefeningen geïncludeerd was, maar niet voor de andere vieze voorwerpen die niet tijdens exposure aan bod waren gekomen. Hetzelfde werd gevonden op het gebied van pijn: exposure-therapie met specifieke gevreesde bewegingen doet de overschatting van pijn door deze specifieke beweging afnemen, maar exposure-therapie leidt niet tot een reductie van het overschatten van pijn voor andere, niet-blootgestelde bewegingen (Crombez et al., 2002; Goubert et al., 2002)1419.
Terugkerend naar voedselcue exposure-therapie concluderen we dat het voor de klinische praktijk belangrijk is dat therapeuten vooraf aan therapie een zorgvuldige analyse dienen te maken van voedingsmiddelen die regelmatig betrokken zijn bij het overeten. De therapeut moet samen met de patiënt zorg dragen dat al deze voedingsmiddelen voldoende aan bod komen tijdens cue exposure-sessies en/of huiswerkopdrachten.
Effect van cue exposure op gewichtsverlies
Om terug te komen op de vraag ‘werkt cue exposure-therapie om gewichtsverlies te bereiken?’ werd in het zojuist toegelichte onderzoek ook gewicht gemeten voor de start van therapie, direct na afloop, en na drie maanden. Op de voormeting hadden proefpersonen gemiddeld een BMI van 33.8, en een gemiddeld gewicht van 96 kilo. Direct na afloop van therapie waren proefpersonen in de cue exposure-conditie gemiddeld meer kilo’s kwijt ten opzichte van hun startgewicht (gemiddeld 2.1 procent, ofwel twee kilo voor de gemiddelde proefpersoon in het huidige onderzoek) dan proefpersonen in de controleconditie (gemiddeld 0.4 procent, ofwel 0.4 kilo voor de gemiddelde proefpersoon). Na drie maanden follow-up was dit verschil nog steeds duidelijk zichtbaar: het behaalde gewichtsverlies in de cue exposureconditie bleef behouden en was nog steeds groter dan in de controleconditie.
Toegegeven, gemiddeld twee kilo in vier weken afvallen is bescheiden, maar als deze dalende lijn zich doorzet, kan op termijn flink wat gewicht verloren worden. Ook is het spannend of het verloren gewicht er ook op de lange termijn vanaf blijft. Per slot van rekening is het afvallen van een aantal kilo’s niet de grootste uitdaging, maar juist het behouden van het gewichtsverlies op de lange termijn.
Desondanks bieden deze bevindingen hoop voor de toekomst. In een onderzoek onder 204 mensen met overgewicht en obesitas bleek dat het toevoegen van cognitieve therapie aan een dieetbehandeling geen acute voordelen had ten opzichte van een dieetbehandeling met een fysieke bewegingscomponent wat betreft gewichtsverlies direct na afloop van de behandeling (Werrij et al., 2009)36. Echter, de groep die naast de dieetbehandeling de cognitieve therapie had gekregen wist het behaalde gewichtsverlies te behouden na één jaar, in tegenstelling tot de andere groep die gemiddeld 25 procent van het startgewicht weer was aangekomen. Gezien de toenemende consensus dat exposure-therapie juist werkt via cognitieve veranderingen (Craske et al., 2008; Hofmann, 2008)1220, zou het zomaar zo kunnen zijn dat de écht boeiende effecten van cue exposure-therapie juist op de langere termijn te observeren zijn in de vorm van terugvalpreventie. Hier ligt een prachtige uitdaging voor toekomstig onderzoek.
Werkingsmechanismen
Naast het vraagstuk over de effecten van cue exposure-therapie, zijn wij ook erg geïnteresseerd in de werkingsmechanismen. Alle cue exposure-studies tot dusver gepubliceerd richten zich op het dalen van trek tijdens cue exposure-sessies, ofwel habituatie van trek. In de angstliteratuur werd inderdaad lang aangenomen dat de habituatie van angst tijdens exposure-sessies essentieel is voor het succes van exposure. De aanname was: hoe sterker angstdaling binnen exposure-sessies, en hoe minder hoog de pieken van angst tussen exposure-sessies, hoe beter het behandelsucces (Foa & Kozak, 1986; Foa & McNally, 1996)1718. Onderzoek heeft echter laten zien dat ondanks veel patiënten habituatie van angst ervaren gedurende exposure-therapie, de mate van habituatie niet samenhangt met beter behandelsucces (Craske et al., 2008). In plaats van het richten op de habituatie van angst, zouden exposure-sessies gericht moeten zijn op het schenden van verwachtingen over het plaatsvinden van de gevreesde uitkomst, zoals een hartaanval in het geval van een paniekstoornis (Craske et al., 2014)13. Een exposure-sessie is volgens deze nieuwe benadering gelukt wanneer de patiënt niet meer, of minder sterk, verwacht dat hij een hartaanval krijgt, en dus niet wanneer de angst voldoende is gezakt. Hoe sterker de discrepantie tussen de verwachting en de daadwerkelijke uitkomst van een exposure-sessie, namelijk dat de verwachtte hartaanval niet optreedt, hoe sterker het leereffect en dus het behandelsucces (Craske et al., 2014). Verwachtingen zouden ook een belangrijke rol in voedselcue exposure kunnen spelen, zoals de verwachting dat het zien en ruiken van lekker eten leidt tot het verliezen van controle over het eetgedrag.
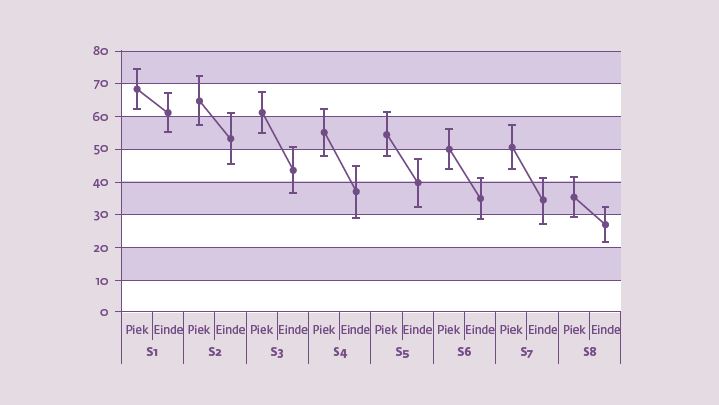
Om te onderzoeken of deze bevindingen in de angstliteratuur ook zo werken voor cue exposure-therapie, namen wij in onze onderzoeken metingen mee om zowel habituatie van trek gedurende exposure-sessies, als de verwachtingen over controleverlies vóór en na therapie te meten. In de laatstgenoemde studie gaven proefpersonen in de cue exposureconditie iedere minuut aan hoeveel trek ze ervaarden op een lijn van 0 mm (helemaal geen trek) tot 100 mm (zeer veel trek). In de analyses werd specifiek gekeken naar het verschil tussen de piek en de eindscore van trek binnen iedere sessie, en het verschil tussen de pieken tussen exposure-sessies: hoe groter de verschillen, hoe sterker de habituatie.
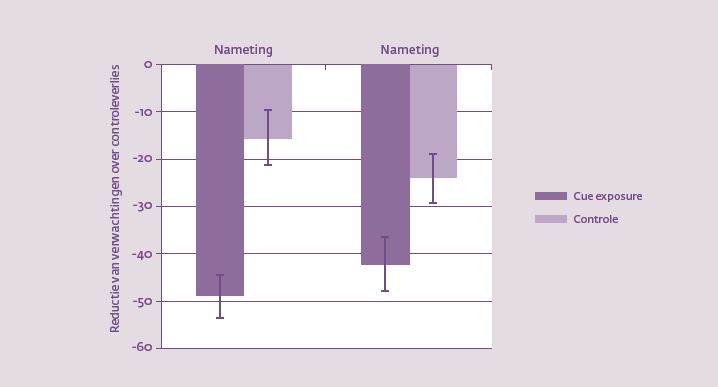
Daarnaast beoordeelden proefpersonen vóór en na therapie de sterkte van verwachtingen over controleverlies bij voedselcues. Voorbeelden van beoordeelde verwachtingen waren: ‘Als ik lekker eten voor mijn neus heb, dan kan ik er niet vanaf blijven’ en ‘Als ik een klein hapje van mijn favoriete snack heb genomen, dan kan ik niet meer stoppen’. Vervolgens onderzochten we het verband tussen habituatie van trek en inname van snacks tijdens de smaaktest. Zoals weergegeven in figuur 2 ervaarden proefpersonen een behoorlijke daling van trek gedurende de cue exposure-sessies, en ook werden de pieken over de sessies heen steeds minder hoog. Maar: de sterkte van habituatie van trek tijdens en tussen exposure-sessies hing niet samen met minder snackconsumptie. De daling van verwachtingen over controleverlies daarentegen, die beduidend sterker waren in de cue exposure conditie dan in de controleconditie (figuur 3), hing wél samen met snackinname.
Deze bevindingen vonden wij ook terug in onze andere cue exposure-studies, en impliceren dat de habituatie van trek – net zoals de habituatie van angst bij angststoornissen – geen belangrijke leidraad is voor cue exposure-sessies. In plaats van het focussen op de daling van trek, zouden cue exposure-sessies gericht moeten worden op het schenden van irrationele verwachtingen over controleverlies. De therapeut zou samen met de patiënt moeten onderzoeken welke cues de verwachting van controleverlies optimaal uitlokken, om vervolgens te testen of het verwachte controleverlies daadwerkelijk plaatsvindt.
Conclusie
Het ‘groeiende’ aantal mensen met overgewicht en obesitas vraagt dringend om effectieve interventies. In de gepresenteerde onderzoeken blijkt cue exposure-therapie succesvol te leiden tot minder overeten, althans voor voedingsmiddelen die tijdens cue exposure-sessies aan bod zijn gekomen.
Generalisatie van cue exposure-effecten naar andere, niet-blootgestelde voedingsmiddelen werd niet gevonden, en suggereert dat het voor de klinische praktijk van belang is om zoveel mogelijk essentiële voedingsmiddelen te betrekken tijdens cue exposure-therapie.
Verder blijkt cue exposure therapie vooral te helpen door voedingsmiddelen te gebruiken die controleverlies uitlokken. Het gebruiken van algemeen ‘lekkere’ voedingsmiddelen lijkt voor minder sterke effecten te zorgen, en therapeuten zouden daarom secuur bij de individuele patiënt moeten nagaan welke precieze producten niet mogen ontbreken tijdens cue exposure-sessies.
Wat betreft de werkingsmechanismen van cue exposuretherapie blijkt dat, in lijn met recente bevindingen in de angstliteratuur, habituatie van trek niet samenhangt met overeten, terwijl een sterkere reductie van verwachtingen over controleverlies wél samenhangt met overeten. Deze bevindingen impliceren dat de daling van trek niet het doel zou moeten zijn van cue exposure-sessies, maar dat de patiënt gedurende de sessie moet leren dat hij de controle niet verliest.
Ten slotte blijken effecten van cue exposure-therapie op overeten ook te vertalen naar gewichtsverlies. Toekomstig onderzoek zal moeten uitwijzen of deze effecten op gewichtsverlies ook op de langere termijn blijven bestaan; tot nu toe kunnen we concluderen dat cue exposure-therapie op de korte termijn helpt om in ieder geval heel wat onsjes minder te wegen.
Met dit artikel won zij de tweede prijs in de Publicatieprijs 2017 van De Psycholoog.